The ambulance service for Brighton and Hove has been rated inadequate and placed in special measures after an official inspection.
The South East Coast Ambulance Service took too long to answer calls, was not safely staffed, did not keep equipment safe and secure and had poor safeguarding procedures.
Poor leadership was also identified by inspectors from the Care Quality Commission (CQC), with the 111 triage scandal given as an example, along with claims of bullying and harassment of staff.
The 111 triage scandal involved delaying calls for help to the 111 phone number, purportedly to ensure the right help was given but also, many suspect, to improve the appearance of the trust’s performance.
Frontline staff won praise though for providing good care to patients.
The official watchdog said today (Thursday 29 September) that the chief inspector of hospitals had recommended that the ambulance trust be placed in special measures.
As a result its policies, procedures and spending will all be subject to greater scrutiny by senior NHS officials.
The damning verdict on the trust comes a month after Brighton and Sussex University Hospitals NHS Trust, which runs the Royal Sussex County Hospital, was also rated inadequate and placed in special measures.
Today the GMB called for the interim ambulance trust chief executive Geraint Davies to be replaced.
This looks unlikely as Mr Davies was brought in when the previous chief executive Paul Sutton and chairman Tony Thorne quit over the 111 triage scandal.
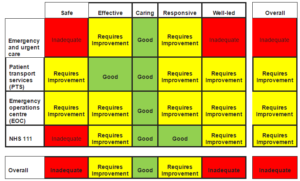
The CQC said: “Overall, the trust has been rated as Inadequate. A team of inspectors rated the service inadequate for providing services that are safe and well led, requiring improvement for being effective and responsive to people’s needs and good for delivering services that are caring.
“A full report has been published at: http://www.cqc.org.uk/provider/RYD.
“During the inspection CQC looked in detail at the trust’s emergency operations centres, the emergency and urgent care service, patient transport services and the NHS 111 service.
“Following the inspection CQC issued a warning notice to the trust identifying six main areas of concern
• The systems in place to ensure enough staff are deployed appropriately were not effective. The trust was not meeting national performance targets for response times. Low staffing levels were having an impact on both performance and fatigue of staff. The trust did not have access to information to review the mix of staff or safe staffing levels.
• NHS 111 calls were not always responded to in a timely and effective manner. While the trust recognised that their performance in meeting the expected standards was not good enough, they had only identified limited actions to improve their performance. When these failed to provide the necessary results there was a lack of strategic leadership.
• Processes to ensure that equipment is properly maintained and secured were not adequate.
• Safeguarding arrangements within the trust were weak. Inspectors found that managers were unclear about their role in safeguarding, including when allegations were made against staff. There was a lack of accountability, and investigation which in turn meant that the trust leadership had a poor understanding of safeguarding issues.
• The systems in place were not operated safely and effectively. The trust had allowed staff to develop practice outside national guidelines which put people using the service at risk
• Governance arrangements including systems to assess, monitor and improve the quality and safety of the services are not operated effectively.”
Professor Sir Mike Richards, Chief Inspector of Hospitals, said: “South East Coast Ambulance Service NHS Foundation Trust has been through a period of significant upheaval following changes in its senior leadership.
“It is to the credit of the staff that they have continued to provide a vital service to the people of Kent, Surrey and Sussex – dealing with almost a million emergency calls a year alone.
“Throughout our inspection we heard how staff were giving their best, treating patients kindly, with dignity, care and compassion.
“It was apparent that the leadership had not been supporting staff to do their jobs effectively. Staff told us there was a culture of harassment and bullying.
“We found in many cases there weren’t enough properly trained staff, or that the proper equipment wasn’t available to them.
“At the time of the inspection, we found evidence that senior executives were not always pulling in the same direction.
“However, improvements are being formulated by an experienced interim chair and the executive has been recently strengthened by new appointments.
“While we have significant concerns about the performance of the ambulance service, I want to provide some reassurance.
“Once care arrives, it is of a good standard – with dedicated and caring call handlers, ambulance crew, paramedics and other frontline staff working hard to ensure this.
“Secondly, the trust are taking urgent steps needed and some improvements have already been made – to ensure that everyone who relies on this service receives excellent, timely care.
“I am recommending that South East Coast Ambulance Service NHS Foundation Trust be placed into special measures to ensure the service gets the support it needs to improve.
“I hope that support from external partners including the NHS Improvement and NHS England will give the trust a clearer sense of direction and support the introduction of the improvements which are so clearly needed.”
The report identifies 13 main areas for improvement
• Governance systems must be effective and fit for purpose. This includes systems to assess, monitor and improve the quality and safety of services.
• The trust must take action to improve the reporting of low harm and near miss incidents.
• The trust must take action to meet national performance targets. .
• There must be improved outcomes for patients who receive care and treatment
• The trust must take action to manage the risk of infection, including ensuring consistent standards of cleanliness in the ambulance stations, vehicles and staff hand hygiene practices.
• There must always be enough staff and managers to meet patient safety and operational standards requirements. This should include ensuring there are adequate resources for staff to usually take their meal breaks, finish on time, and undertake administrative and training.
• The trust must recruit enough Hazardous Area Response Team (HART) paramedics to meet its requirements under the National Ambulance Resilience specification.
• The trust must ensure that ambulance crews’ qualifications, experience and capabilities are taken into account when allocating crews to ensure that patients are not put at risk from inexperienced and unqualified crews working together.
• The trust must take action to protect patients from the risks associated with the unsafe use and management of medicines. This should include: appropriate use of patient group directives; the security and safe storage of both medicines and controlled drugs; the management of medical gas cylinders.
• Patient records must be completed appropriately, kept confidential and stored securely. The trust must take action to ensure that all staff working with children, young people and/or their parents/carers receive an appropriate level of safeguarding training.
• The trust must ensure all Emergency Operations Centre premises containing confidential data and critical equipment are secure. Take action to ensure the Computer Assisted Despatch CAD system is properly maintained.
• Every operational member of the Hazardous Area Response Team must have a minimum of 37.5 hours protected training time every seven weeks.
• There must be a contingency plan to deal with the loss of the patient transport services control room in Dorking that will allow the service to continue.
The inspection team also highlighted areas of good practice including
• The trust encouraged staff to take on additional roles and responsibilities and provided training and support to enhance the paramedic roles.
• The trust worked well with commissioners and local stakeholders to meet the needs of the local population. This included working with GPs in community settings and patients’ own homes.
• Patients were supported to manage their own health by using non-emergency services such as their GP, local urgent care centres or alternative care pathways when it was appropriate to do so.
Yesterday (Wednesday 28 September) the CQC was due to presented its findings to a local quality summit, including NHS commissioners, providers, regulators and other public bodies. The purpose of the quality summit was to develop a plan of action and recommendations based on the inspection team’s findings.






